|
The spectrum of changes in renal size, contour, and pelvicalyceal system is summarized in ( Figure 64-11 ). The causes of bilateral renal enlargement include infiltrative processes and infectious and immune disorders, most of which consist of glomerular diseases (see Figure 64-10 ). Diffuse unilateral nephromegaly also may be seen when physiologic compensatory hypertrophy occurs in the setting of contralateral renal failure. Unilateral diffuse nephromegaly may be secondary to renal edema from renal vein thrombosis or urinary obstruction. ADPKD, Autosomal dominant polycystic kidney disease ARPKD, autosomal recessive polycystic kidney disease HIV, human immunodeficiency virus JG, juxtaglomerular MCDK, multicystic dysplastic kidney disease MLCN, multilocular cystic nephroma PCS, pelvicalyceal system SLE, systemic lupus erythematosus TCC, transitional cell carcinoma VHL, von Hippel-Lindau syndrome XGP, xanthogranulomatous pyelonephritis. Diseases that cause renal cortical atrophy also may result in compensatory renal sinus lipomatosis with little alteration in bipolar renal length ( Figure 64-9 ).Īlgorithm showing approach to diffuse renal parenchymal diseases with increase in renal bulk. Further differentiation is limited in this subgroup except determination if the process is unilateral or bilateral (see Figure 64-7 ). No focal scars or calyceal papillary distortions are noted. Smoothly marginated, small kidneys are seen in diseases that cause tubular atrophy and fine interstitial fibrosis. Of these, only renal infarction will not cause any underlying calyceal abnormality ( Figure 64-8 ). Contour irregularity is seen with renal infarction, reflux nephropathy, and advanced analgesic nephropathy. The finding of small kidneys therefore implies that chronic diffuse renal disease is present.ĭiseases that manifest as small kidneys are further categorized into those with smooth or irregular contour ( Figure 64-7 ). Thus, prior or serial ultrasound evaluation may be of greater benefit than a single measurement. Disease processes may initially cause an increase in renal size as a result of acute-phase edema and then cause a chronic decrease in renal size as a result of fibrosis. Renal size varies considerably within populations and by gender from 10 to 14 cm in males and 9 to 13 cm in females. 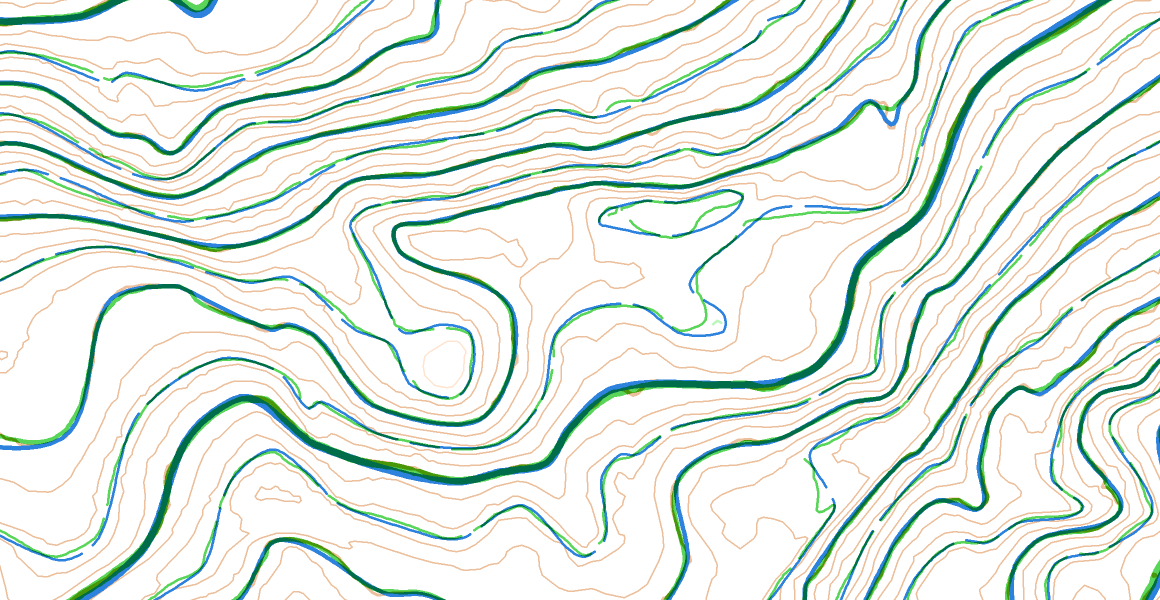
Renal size should be assessed in all patients. Radiologic approach to renal parenchymal diseases. Apparent expansion of the renal sinus fat is a commonly seen secondary sign of diffuse atrophy due to chronic renal diseases ( Figure 64-1 ). The kidneys may show poor contrast excretion, depending on the stage of renal failure. 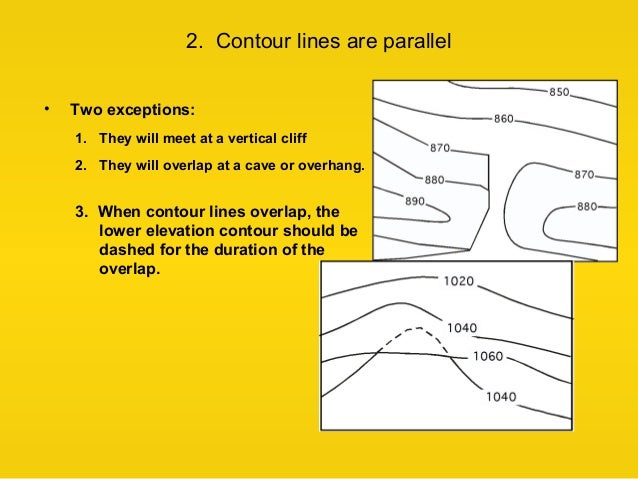
Intravenous urography may show bilaterally smooth, enlarged or small kidneys. Newer techniques such as diffusion- and perfusion-weighted imaging and ultrasmall superparamagnetic iron oxide (USPIO)-enhanced imaging may have advantages when evaluating diffuse renal diseases by not requiring a biopsy. Magnetic resonance imaging (MRI) is insensitive to urinary stones and nephrocalcinosis, but it is useful in the imaging of renovascular abnormalities. Contrast-enhanced CT, as with IVP, requires nephrotoxic iodinated contrast and therefore is typically not used if renal function is abnormal. Noncontrast computed tomography (CT) is useful for visualizing stones and the distribution of nephrocalcinosis. Excretory or intravenous pyelography (IVP) (requires the administration of potentially nephrotoxic iodinated contrast and is therefore generally not performed in patients with diffuse renal parenchymal disease. Morphologically the kidneys show a smooth contour. The kidneys may be enlarged in acute GN or may be small in chronic GN. Ultrasonography also may demonstrate calculi and nephrocalcinosis. Ultrasound evaluation of the kidneys is useful to exclude other causes of renal function impairment. 
Pathologic and immunologic assessment of biopsy samples continues to be the mainstay in diagnosis. Glomerulonephritis (GN) has no specific imaging findings. These conditions are discussed in this section. Renal parenchymal abnormalities may be divided into those that involve the entire kidney, such as rejection, glomerulonephritides, amyloidosis, and drugs, and those that are either primarily cortical or primarily medullary, such as nephrocalcinosis. Postrenal causes of abnormal renal function are typically those causing obstruction to the urine outflow from calculi, ureteropelvic dysfunction, or masses. Renal vein thrombosis results in increased backpressure and edema. 
Renal artery stenosis results in decreased perfusion. Prerenal renal failure may arise from alterations in renal artery perfusion or venous drainage. Renal failure may be classified as prerenal when secondary to a reduction in the renal perfusion pressure gradient, renal when the result of intrinsic disease of the renal parenchyma, and postrenal when secondary to an abnormality of urine outflow.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
